May-Thurner Syndrome (MTS) is a medical condition where the left iliac vein, responsible for carrying blood from your lower half back to your heart, is compressed by the right iliac artery.
This pressure can lead to various issues in the left leg, such as pain, swelling, and the appearance of varicose veins. In more severe cases, it could lead to deep vein thrombosis (DVT), a critical ailment in which a blood clot develops in the veins deep inside your body.
As experts in vein disease with more than a decade of experience, we at the Texas Vascular Institute are here to shed light on MTS diagnosis, treatment, and prevention.
The Origins of May-Thurner Syndrome
To understand the cause of MTS, it’s crucial to explore the anatomy of the iliac veins. These large veins cross over each other in the pelvis – the right iliac vein running above the left.
This can sometimes lead to the right iliac artery, which pulsates with each heartbeat, compressing the left iliac vein beneath it. The resulting pressure can impede blood flow in the left leg, causing the symptoms associated with MTS.
Several risk factors can increase your likelihood of developing MTS:
- Gender: Women are more likely to experience MTS.
- Age: It’s more prevalent in the 20-40 age group.
- Pregnancy: The increased blood volume and hormonal changes during pregnancy can put extra pressure on the iliac veins.
- Obesity: Extra weight can increase pressure on the veins in the pelvis.
- Sedentary Lifestyle: Lengthy periods of sitting or standing can exacerbate vein issues.
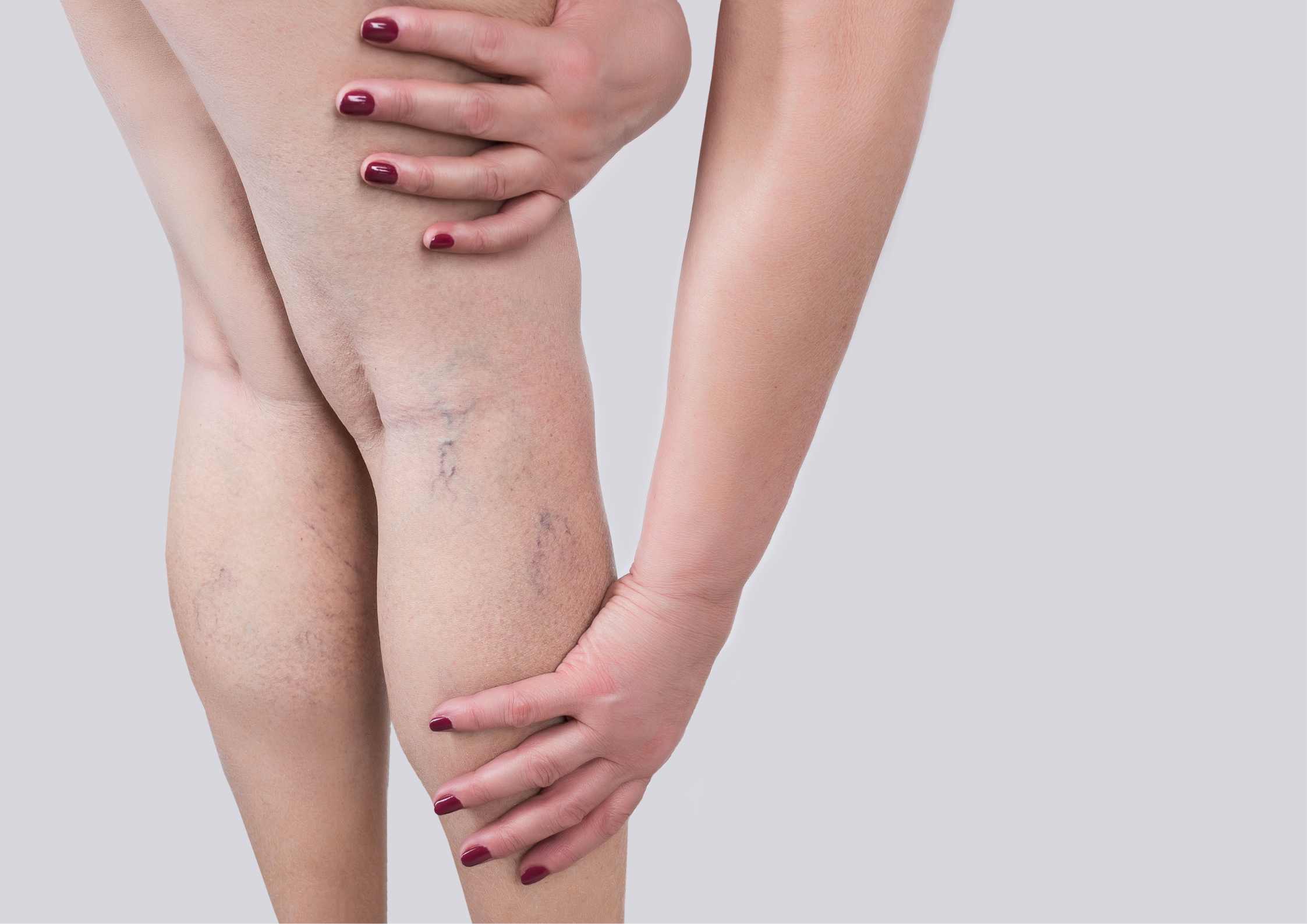
May-Thurner Syndrome and Women’s Health
MTS is often associated with other conditions affecting women’s health. For instance:
- Uterine Fibroids: These are non-cancerous growths in the uterus, causing heavy bleeding, pelvic pain, and in some cases, infertility.
- Pelvic Venous Congestion: This involves the dilation of ovarian veins and other veins in the pelvis, resulting in chronic pelvic pain, varicose veins, and discomfort in the vulvar region.
- Pregnancy: The hormonal changes and increased blood volume during this period can heighten the risk of developing MTS or DVT.
We diagnose these conditions using various techniques and offer minimally invasive procedures for treatment. Some of these treatments include:
- Uterine fibroid embolization: This procedure involves blocking the blood supply to the fibroids, causing them to shrink over time.
- Pelvic venous congestion embolization: This treatment method blocks the refluxing of ovarian veins, alleviating the symptoms associated with this condition.
- Anticoagulation therapy: Often recommended during and after pregnancy, this involves the intake of blood thinners to prevent clot formation.
As specialists in treating vein conditions, we’re committed to providing the most effective treatment options to help our patients lead healthier, happier lives.
Diagnosing May-Thurner Syndrome
MTS can be a tricky condition to diagnose because it often goes unnoticed until a more severe complication, like deep vein thrombosis (DVT), arises.
However, various tests can detect MTS early and effectively. These include ultrasound, venography (an X-ray of the veins), magnetic resonance imaging (MRI), and computed tomography (CT) scans.
If you notice signs or symptoms of MTS or DVT—like swelling, pain, or varicose veins in your left leg—it’s crucial to seek medical attention promptly.
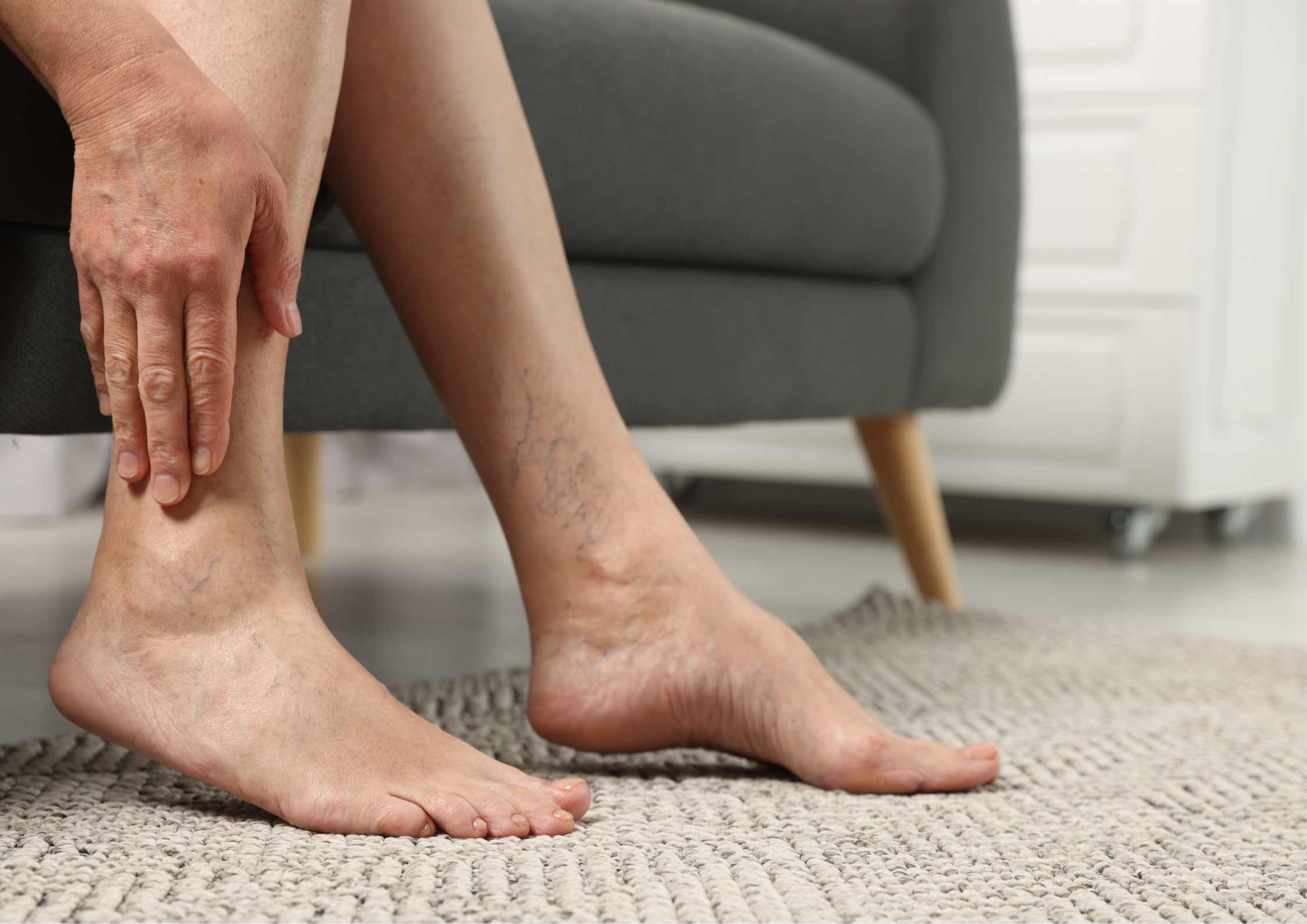
Treating May-Thurner Syndrome
When it comes to treating MTS, the primary goals are to alleviate symptoms, restore blood flow, and prevent complications. Various treatment options are available, each with its own unique advantages:
- Medications: Anticoagulants, or blood thinners, can prevent clotting and reduce inflammation in the affected vein.
- Compression Stockings: These elastic garments exert pressure on the legs, aiding in better circulation.
- Endovascular Procedures: These minimally invasive techniques use catheters and devices to widen the narrowed vein and remove clots. Examples of these procedures include:
– Angioplasty: a balloon is inflated inside the vein to widen it.
– Stenting: a metal mesh tube is inserted inside the vein to keep it open.
– Thrombolysis: clot-dissolving drugs are injected into the vein.
– Thrombectomy: clots are removed using a suction device or a mechanical tool.
Endovascular procedures offer numerous benefits:
- High success and low complication rates.
- Short recovery times with minimal scarring.
- Procedures are performed under local anesthesia and sedation.
- Most procedures are covered by insurance plans.
At the Texas Vascular Institute, our team is well-versed in performing these endovascular procedures for MTS and other vein conditions.

Preventing May-Thurner Syndrome
While there’s no definitive way to prevent MTS, certain lifestyle changes can minimize the risk of developing it or exacerbating existing symptoms:
- Maintaining a healthy weight and diet reduces pressure on the pelvic veins.
- Regular exercise aids in improving overall circulation.
- Avoid prolonged sitting or standing, as frequent movement helps prevent blood pooling in the legs.
- Elevating your legs when resting or sleeping can facilitate blood flow back to the heart.
- Wear compression stockings, if advised, which assist in improving blood flow.
- Quit smoking and limit alcohol since both are known to affect circulation negatively.
By adopting these changes, you can lead a healthier life and significantly reduce the chances of developing or worsening MTS.
Frequently Asked Questions and Myths About
May-Thurner Syndrome
As a clinic specializing in vein diseases, we often encounter a variety of questions about MTS and its treatment. Here are answers to some of the most frequently asked questions:
How common is MTS, and who is at risk?
MTS is more common among women aged 20-40, but it can affect anyone, regardless of age or gender. Factors like pregnancy, obesity, and a sedentary lifestyle can increase the risk.
How can I prevent MTS or DVT from happening?
Making necessary lifestyle changes, such as maintaining a healthy weight, engaging in regular physical activity, and avoiding prolonged sitting or standing, can provide significant benefits.
What are the potential complications or side effects of MTS treatment?
As with any procedure, there’s a risk of complications, such as infection or bleeding. However, our modern, minimally invasive treatments have low complication rates.
How long does it take to recover from MTS treatment?
Recovery time varies, but generally, patients recover from endovascular procedures within a few days to a week.
Will I need to take blood thinners for life after MTS treatment?
Not necessarily. Your doctor will determine the duration of your medication based on your condition and treatment.
Despite the information available about MTS, there are still several misconceptions that persist:
Myth #1: MTS only affects older people or those with other health problems.
Fact: MTS can affect anyone, although certain factors like gender and age can increase risk.
Myth #2: MTS is not a serious condition and does not need treatment.
Fact: MTS can lead to severe complications like DVT if left untreated.
Myth #3: MTS treatment is painful, risky, or expensive.
Fact: Modern MTS treatments are minimally invasive, have high success rates, low risk, and are covered by most insurance plans.
Myth #4: MTS treatment will cure the condition permanently.
Fact: While treatment can relieve symptoms and restore blood flow, ongoing management may be necessary to prevent recurrence.
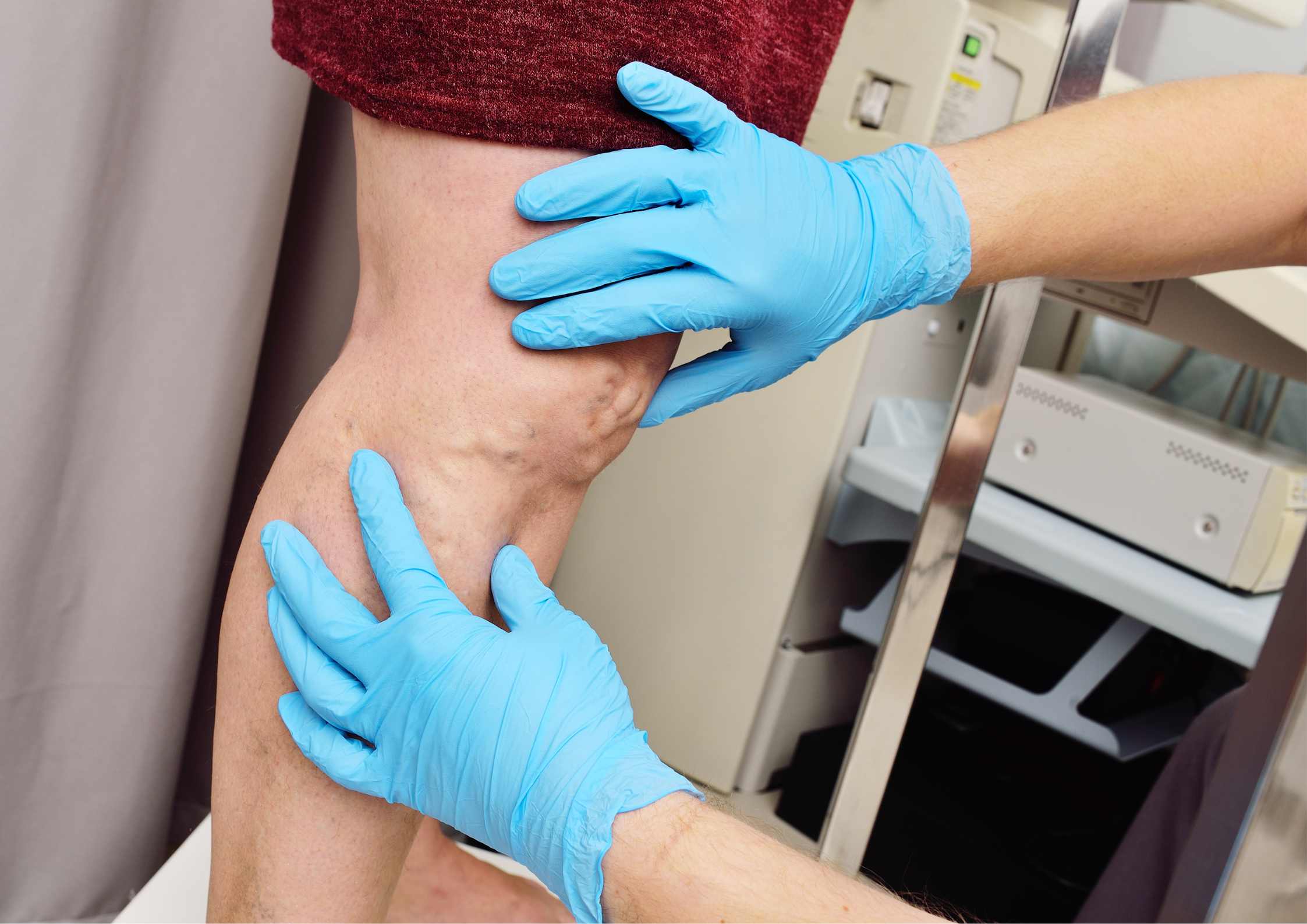
In Summary
MTS is a serious condition that affects the veins in the left leg, leading to symptoms like pain and swelling and potentially causing life-threatening complications like DVT. Diagnosis includes methods such as ultrasound, venography, MRI, and CT scans.
Treatment goals are to relieve symptoms, restore blood flow, and prevent complications, with options ranging from medications and compression stockings to minimally invasive endovascular procedures.
While there’s no definitive prevention method for MTS, certain lifestyle changes can minimize your risk or manage symptoms if you’re already diagnosed with the condition.
If you have further questions or concerns about MTS or other vein conditions, the Texas Vascular Institute team is here to help. To schedule an appointment or consultation, don’t hesitate to contact us at 972-798-4641 or visit our website.
Don’t let vein disease affect your quality of life—reach out to our expert team today!
WHAT OUR PATIENTS
have to say
Texas Vascular Institute always appreciates feedback from our valued patients. To date, we’re thrilled to have collected 378 reviews with an average rating of 5 out of 5 stars. Please read what others are saying about Texas Vascular Institute below, and as always, we would love to collect your feedback.
Leave a Review
Amazing Practice
I'm very particular with my Healthcare and tend to be cautious with referrals to specialists. This office is amazing from the first point of contact. Their staff are friendly, professional and highly knowledgeable. Then the Dr is just as amazing as his staff, absolutely brilliant. Office manager Jessica has this office running like a well oiled machine and does so with a smile, an air of confidence, kindness and professionalism. Love this practice!!
- Richard G.

Beyond Thankful
Dr Batra and his staff are amazing! We are so grateful to have found him. Everyone is so kind and so caring and Dr Batra explains everything so well and does procedures with excellence. Beyond thankful to be under their care!!!
- Bitsy P.

Gold Standard
This is a gold standard for how a medical practice should be run. I was promptly seen at my scheduled time, my ultrasound was thorough and I received plenty of attention and care from the staff and Dr.Batra.
- Weronika L.
INSURANCE
We accept most major insurance plans. Please contact the medical office for all insurance related questions.








8330 Meadow Rd #100
Dallas, TX 75231
For Appointments: 972-798-4710
General Inquiries: 972-646-8346
809 West Harwood Rd, Suite 101,
Hurst, TX 76054
For Appointments: 972-798-4710
General Inquiries: 972-646-8346
4716 Alliance Blvd Suite #180,
Plano, TX 75093
For Appointments: 972-798-4710
General Inquiries: 972-646-8346

